Osteoarthritis (OA) of the knee
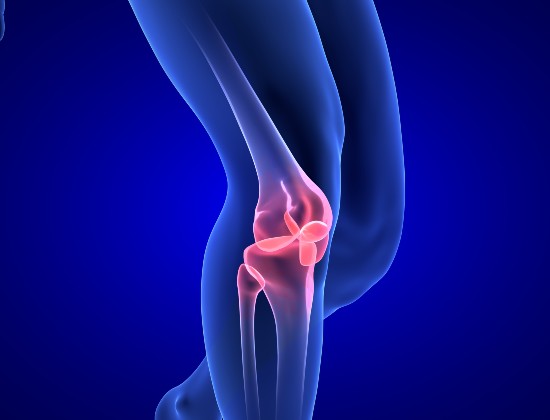
The knee joint consists of the lower end of the thigh bone (femur) and the top of the shin bone (tibia); at the front of the knee is the knee cap (patella). The patella moves up and down in a groove on the front of the femur as the knee bends and straightens.
All the surfaces of the bones are covered in articular (chondral) cartilage, which is a smooth, tough and rubbery surface that allows the bones in the knee joint to move easily against each other with minimal friction.
The bones are held together by ligaments and joint capsules; the meniscal cartilages help load-sharing and stability in the medial (inner) and lateral (outer) portions of the joint between the shin bone (tibia) and thigh bone (femur).
What is osteoarthritis of the knee?
Osteoarthritis (OA) of the knee is the most common form of arthritis, causing pain, swelling and stiffness. It’s caused by long term wear to the joint surface cartilage. Thanks to recent research into the causes of knee OA and its treatment, doctors are now able to offer a more effective approach to the management of this condition.
Which areas of the knee are affected?
The most commonly affected areas of the knee are the medial and patellofemoral compartments:
- The medial compartment is the inner side of the knee, between the thigh and shin bones
- The patellofemoral compartment is between the kneecap and the thigh
- The lateral compartment is the outer side of the knee, between the thigh and shin bone
How is it caused?
- OA is usually a slow, progressive process of wearing of the joint cartilage and is therefore more common in older patients (as joint surface cartilage wears out, raw bone may eventually be exposed)
- It is more likely if you have particular inherited traits that put more pressure on the joints, for example bowed legs
- It can also affect people after they have had an injury either directly to the joint surface or to surrounding ligaments, for example an anterior cruciate ligament (ACL) injury
What are the symptoms?
- Pain, swelling, stiffness and limited movement of the knee joint
- Stiffness in the knee(s) first thing in the morning or after sitting for prolonged periods of time
- Stiffness is often eased with gentle activity such as walking, although in more severe cases even short walks can be painful
- Sometimes the knees ‘creak’ or ‘crunch’ when you walk or squat. This can be a symptom of knee OA, although this is not always the case as healthy knee joints make these noises too!
Some people may have very advanced OA damage and feel very little pain, while others may have severe pain but with very little wear of the joint showing on an X-ray. When knee OA symptoms are very advanced, they can have a major impact on all areas of your life including gentle exercise such as walking, and it can also affect sleep quality.
How is it diagnosed?
A diagnosis made during a medical consultation is usually backed up by X-rays that will show the extent of the damage. You may also be offered an MRI scan, if the diagnosis is not clear, to differentiate knee OA from other conditions, such as a meniscus tear.
How is it treated?
Your treatment will depend on a number of factors, including the physical, social and emotional effects that the condition is having on your life.
Non-operative treatments: these may include painkillers or anti-inflammatory medication, physiotherapy, exercises to improve your strength and fitness, and acupuncture. Injections with viscosupplements (a synthetic form of the synovial fluid that is naturally produced in the joint) may also be helpful. Maintaining a healthy body weight by keeping to a balanced diet and taking regular low impact exercise, for example cycling and swimming, are also important to help maximise the health of your knee(s) and prevent further joint deterioration. OA is more likely to progress in people who are obese, and are therefore putting much more load on their knees, than in people who are of a healthy weight.
Surgery: in advanced cases, where non-operative treatments have not helped, a knee replacement may be the only option. During this procedure either the whole of the joint is replaced, known as a total knee replacement (TKR), or only one half, known as a unicompartmental knee replacement (UKR). However, there are also other surgical procedures which can be very effective in the treatment of less advanced forms of OA. For example, the realignment (straightening) of an arthritic knee (during an osteotomy) is now a very reliable procedure for some patients and may avoid the need for a knee replacement, or at least delay it for many years.
Important: This information is only a guideline to help you understand your treatment and what to expect. Everyone is different and your rehabilitation may be quicker or slower than other people’s. Please contact us for advice if you’re worried about any aspect of your health or recovery.











.png)









.png)