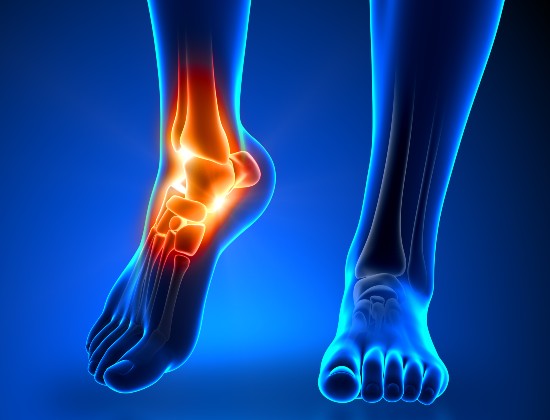
Achilles tendon pain and tendinitis
The Achilles tendon is the large tendon found at the back of your ankle. It connects the calf muscle to the heel bone and is important in being able to bring the foot downwards, going on tip-toe, and also providing a good push-off when walking or running.
What causes Achilles tendon pain?
Pain in the Achilles tendon, more common among middle-aged athletes, can be caused by a number of factors, including a rapid increase or change in a training regime. However, in some cases, the tendon can sometimes become painful for no apparent reason, even when someone is in regular training; this may be due to arthritis or other inflammatory disorders.
What happens to the tendon?
The tendon is made up of strong fibres formed of collagen, which become weaker and less flexible over time. As this happens, tiny microscopic tears can develop, leading to weakness, pain and eventually swelling. Swelling is often in the middle of the tendon because this area has a less well-developed blood supply so is unable to heal itself as effectively.
What are the symptoms?
- Pain and stiffness along the Achilles tendon in the morning
- Pain along the tendon or back of the heel that worsens with activity
- Swelling that is there all the time and can become worse throughout the day with activity
- Severe pain the day after exercising
- Thickening of the tendon
What is tendinitis (Achilles tendinopathy)?
This is a commonly used term for anyone with Achilles pain. It’s not strictly accurate, however, because pain is usually caused by tissue degeneration in the tendon fibres (tendinopathy) rather than inflammation (tendinitis) of the tissue. It’s therefore more accurate to use the term ‘Achilles tendinopathy’. There are two types of Achilles tendinopathy:
- Non-insertional: when pain, weakness and loss of function is associated with swelling in the main portion of the tendon and not at the bottom by the heel bone
- Insertional: when pain, weakness and loss of function are associated with a swelling at the bottom of the tendon by the heel bone. Sometimes the heel bone can be quite prominent and very painful. This can be caused by Achilles tendon degeneration, bone spurs (bony lumps), or inflammation of a small bursa (the fluid filled sac behind the tendon), known as bursitis
How is it diagnosed?
A medical examination and discussion of your symptoms can be backed up by an X-ray to show tissue swelling or bone spurs; however, an MRI scan can be more effective as it shows the tendon quality in more detail.
Can the problem become worse?
People often put up with the symptoms for some time, or alter their level of activity, before seeking medical advice. However, symptoms can become worse and there can be a rupture of the tendon.
How is it treated?
Non-operative treatment: most people with tendinopathy don’t need to have surgery. Reducing your level of activity, resting, and taking anti-inflammatory medication and painkillers (if advised by your doctor) along with physiotherapy can really make a difference. You may be advised to use a small silicone insert in your shoe to raise your heel and, in some cases, shockwave therapy may also be recommended.
Surgery: if the tendon does not recover, you may be offered surgery to explore the painful tendon area and remove any damaged or inflamed tissue, or painful bony bumps on the heel. If the tendon is detached from the bone during surgery or a large amount of the tendon is removed, then tendon replacement surgery using another tendon in the foot to support the damaged Achilles tendon may be needed.
Important: This information is only a guideline to help you understand your treatment and what to expect. Everyone is different and your rehabilitation may be quicker or slower than other people’s. Please contact us for advice if you’re worried about any aspect of your health or recovery.