Coccydynia
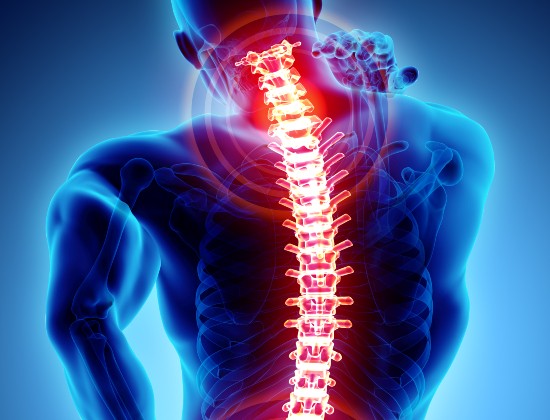
Coccydynia is pain in the coccyx (the last bone in the tail of the spin), which is usually worse when you are sitting down. The coccyx consists of three bones which are loosely joined and help to take your weight when you are sitting.
Coccydynia causes only around one per cent of lower back pain although women are five times more likely to have the condition, as it can develop when they are giving birth. Older people are also more likely to have the condition, due to wear and tear on the discs around the coccyx or the bones becoming fused.
Causes
Pain in the coccyx can be caused by:
- Damage to the muscles and ligaments around it (for example, during childbirth)
- Landing heavily on it (for example, during skiing or ice skating, or falling from a horse)
- Repetitive strain injury from repeated activity (such as rowing or cycling)
- Poor posture
- Being overweight or underweight (if you are overweight you can put more pressure on the coccyx when you are seated; if you are underweight the the coccyx can rub on tissues around it)
- Age-related wear and tear (where there is no other obvious cause)
Symptoms
Pain, especially while you are seated or when you get up from a chair is the most common symptom. You may also have sharp pains in your legs, pain in other areas of your back, and in your buttocks and hips.
Diagnosis
Usually coccydinia can be diagnosed during a discussion of your symptoms and a medical examination, although in some cases you may be offered X-rays while you are sitting and standing to find out if the coccyx is moving more than it should and to check for fractures.
Treatment
Non-operative treatment: this may include anti-inflammatory medicine, if advised by your doctor. In some cases you may also be offered physiotherapy, and spinal injections such as steroids to reduce pain and inflammation.
Surgery: in some cases, if you are still in a great deal of pain, you may be offered a coccygectomy. This procedure is carried out under a general anaesthetic and involves removing the coccyx, reattaching the muscles, tendons and ligaments around it to the pelvis. After surgery, 80-90 per cent of people will have improved symptoms, although this can take around three months.
Important: This information is only a guideline to help you understand your treatment and what to expect. Everyone is different and your rehabilitation may be quicker or slower than other people’s. Please contact us for advice if you’re worried about any aspect of your health or recovery.