Midfoot arthritis
The midfoot is the section of the foot that begins at the level of the Chopart joint. It consists of five bones, connected to each other and to the hindfoot and forefoot. The bones are known as: cuboid, navicular, medial, intermediate and lateral cuneiform bones. The midfoot ends at the Lisfranc (or tarsometatarsal) joint, where the metatarsal bones begin.
What causes midfoot arthritis?
There are different reasons for developing arthritis in the small joints in the midfoot. These include:
- Post-traumatic - Bone fracture or damage/dislocation at any of the bones or joints, even if successfully treated many years before
- Rheumatoid arthritis - Patients with rheumatoid or other forms of inflammatory arthritis can also develop arthritis in their foot
- Osteoarthritis - Even where there is no injury, arthritis can develop without explanation in the midfoot
- Tibialis posterior tendon dysfunction - If this tendon in the foot develops problems then the arch can flatten and you can develop midfoot or hindfoot arthritis
What are the symptoms?
- Aching in the middle of the foot when walking/activities
- Loss of flexibility in the foot, especially on uneven surfaces
- Swelling on the top of the foot that can sometimes be quite hard and bony
- The foot can change its shape and look flatter, with loss of the natural arch
- Wearing certain shoes can rub on the skin on the top of the foot
People often live with the symptoms for many years before seeking medical help and the pain and stiffness gradually becomes worse. This can make walking and weight-bearing exercise more difficult. Although it can be treated at any stage, nearby joints may be affected as it develops.
Can it become worse?
People often put up with the symptoms for many years before seeking medical advice. If you decide not to see your doctor, the problem will tend to become worse, usually slowly. Stiffness and pain will usually increase, making walking and weight-bearing exercise gradually more difficult. The condition can be treated at any stage but, as it develops, more nearby joints can become affected.
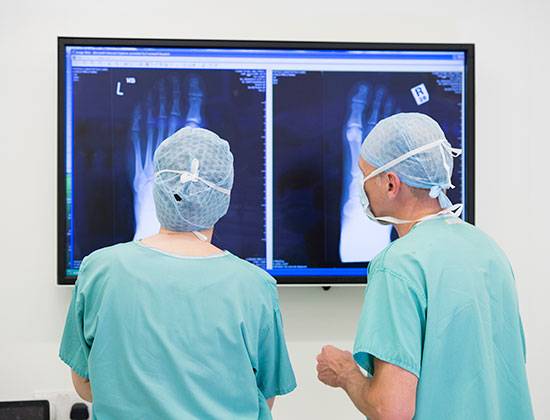
How is it diagnosed?
After a medical examination and discussion of your symptoms, X-rays can confirm the diagnosis. You may also be offered a CT scan to identify exactly the joints involved.
How is it treated?
Treatment can involve a combination of different therapies including:
- Painkillers and anti-inflammatory medication
- Shoe modification: often stiffer soled shoes or rocker-bottom shoes can really help when walking, talking the strain off the painful joints
- Lifestyle advice and avoidance of exercise that make pain worse
- Steroid/anaesthetic injections into the joints every six months, under ultrasound control, which give excellent pain relief
- Physiotherapy to keep your calf muscles relaxed and ensure you don’t overload the foot
- Surgery: this can simply involve removing any bony lumps on the top of the foot but usually involves foot fusion surgery of the small painful joints
Important: This information is only a guideline to help you understand your treatment and what to expect. Everyone is different and your rehabilitation may be quicker or slower than other people’s. Please contact us for advice if you’re worried about any aspect of your health or recovery.