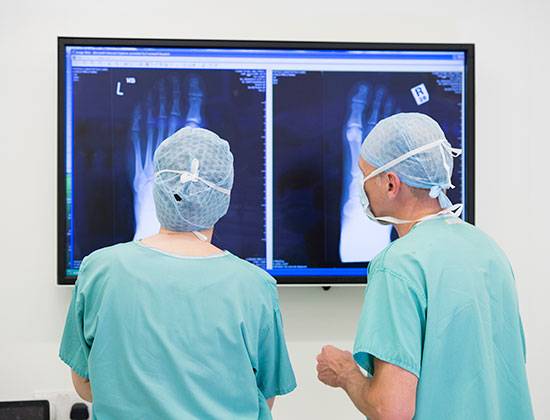
Ankle replacement surgery (arthroplasty)
The ankle joint is the joint at the bottom of your shin bones (tibia and fibula) and the start of your foot bones (the talus bone). Where the bones meet, they are covered by a smooth cartilage lining of the joint which allows you to move the ankle freely.
Who might need an ankle replacement?
In people who have, for example, severe osteoarthritis, rheumatoid arthritis or possibly a previous injury or fracture of the ankle, the cartilage in your ankle joint becomes damaged; gradually the space in your joint narrows, with bone on bone contact causing pain and stiffness and, in some cases, a deformity of the ankle.
What is an ankle replacement?
An ankle replacement is performed to remove the damaged joint lining as described above and replace it with metal components. The metal components are firmly attached to the bones in the ankle (tibia and talus). Movement is achieved by a highly specialised piece of plastic inside the joint.
How is surgery carried out?
You will usually spend one or two nights in hospital. The operation is performed under a general anaesthetic, with an added injection in the leg to numb the foot after surgery. The procedure involves carefully removing the damaged arthritic joint surfaces and replacing them with metal components that are attached to the remaining bone surface.
What to expect immediately after surgery
Your foot will be in a plaster cast to the knee. It will be numb and pain-free. You will see a physiotherapist who will advise on walking while keeping weight off the ankle using crutches. You will be discharged only when you are comfortable, with a follow-up appointment and painkillers as required.
Recovery
During the first few weeks after surgery:
- Elevate your foot as often and as much as possible to reduce swelling
- Some blood ooze can be expected in the bandage. If you are worried, contact the Fortius Clinic for advice
- After two weeks: begin a gentle range of ankle exercises out of the boot as advised by your consultant
- Excellent pain relief within the first few weeks
- Good walking function; able to start building up your activity from around four weeks, with improvement up to 12 months
- Some swelling may remain in your foot and ankle for 6-12 months following surgery
- Walking should be markedly improved and most people return to their normal activities
- Your range of ankle movement may improve with positive outcomes expected in 85-90% of patients continuing up to 10-15 years after surgery
- Loosening/failure of the implant
- Infection
- Nerve damage
- Ankle stiffness
- Continued ankle symptoms
- Deep Vein Thrombosis (DVT)
- Take painkillers as prescribed by your doctor
Follow-up appointments
Everyone is different, so healing and post-operative programmes vary from person to person. However, the follow-up appointments below are typical:
- 2 weeks: wound check and new boot applied
- 6 weeks: remove boot and X-ray
- 12 weeks: X-ray and follow-up appointment
- 6 months: X-ray and follow-up appointment
- 12 months: X-ray and follow-up appointment
- Yearly: X-ray and follow-up appointment
When can I start to walk?
This will vary according to your surgical treatment; typically after simple ankle debridements you can walk with the use of crutches for the first couple of weeks. If you have cartilage repair surgery you may be required to stay non-weight bearing for the first couple of weeks. Weight bearing will be advised by your surgeon, but typically this might be:
- 0-2 weeks: plaster cast, non-weight bear with crutches
- 2-4 weeks: cast/boot, weight bear as advised
- After 4 weeks: full weight bear
Getting back to normal
Your physiotherapist will guide you through the stages of rehabilitation including gait re-education (learning to walk normally again), as well as exercises to reduce swelling and muscle tightness.
- After four weeks: increase the movement and begin resistance exercises as advised, gradually increasing them as you gain strength
How do I wash and shower?
Keep the plaster cast totally dry. You can shower with a waterproof cover over the plaster. Once the plaster is removed you can shower, if the wound is healed, by carefully removing the boot and gently dabbing the wound dry.
How can I look after the operation wound?
Once out of the cast, do not pull at scabs but let them fall away naturally. If your wound becomes red, swollen or sore, contact the Fortius Clinic and arrange to see your consultant to check there is no infection.
When can I start to drive again?
The DVLA states that it is the responsibility of the driver to ensure they are always in control of the vehicle. A good guide is if you can stamp down hard with the foot to stop the car during an emergency stop. Being able to do this can take at least six weeks.
When can I return to work?
This depends on the type of work you do and how quickly you recover. As a general guide, if your job involves sitting down for most of the time, you should be able to return to work after four weeks; if it involves manual work, you may need to have up to twelve weeks off.
What are the risks?
Below is a guide to the risks of this type of surgery. Your surgeon will discuss this with you before your procedure, and answer any questions you may have:
Like any artificial implant, the ankle replacement can loosen. Hip and knee replacements are currently more reliable than ankle replacements with around 15% of ankle patients needing repeat surgery after 10-15 years
Infection is quite rare (less than 1%) but can be difficult to treat if it is deep inside the ankle joint and may require further surgery, possibly to fuse the joint. Your surgeon will be able to discuss this with you before surgery
In around 5% of cases inflammation and synovitus can occur after surgery, which can slow down recovery.
Small nerves that supply sensation to the skin near the operation site can be damaged, although the risk of this is small (less than 5%). If your toe stays numb after surgery, the nerve may be bruised but this will usually recover
Although the operation is designed to retain movement, some patients may not regain full movement. Physiotherapy can help with this
You may continue to have some mild discomfort (around 30% of people are affected). However, the level of discomfort is usually much less than before surgery
DVT (where a blood clot forms in a deep vein in the leg) is unusual after ankle replacement surgery and carries a risk of less than 5%. However, you may be given blood-thinning medication after surgery as a precaution.