Anterior cutaneous nerve entrapment syndrome (ACNES)
What is ACNES?
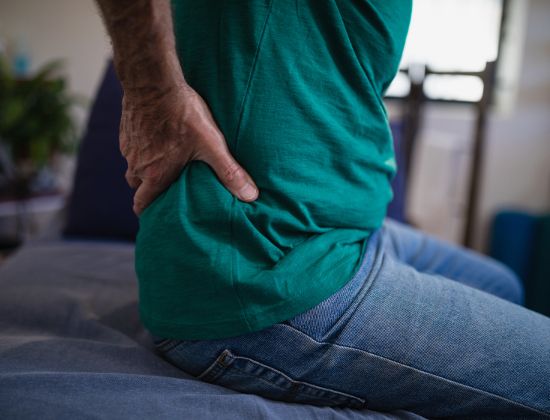
Abdominal Cutaneous Nerve Entrapment Syndrome (ACNES) is one of the now recognised causes of chronic abdominal pain. It remains an overwhelmingly underdiagnosed condition and consequently not readily managed or recognised. It is generally characterised by patients presenting with a severe, often refractory, chronic abdominal pain just lateral (next to) the midline. Often the pain can be pinpointed to a specific location on the abdomen. It is theorised that the cutaneous branches of the lower thoracoabdominal intercostal nerves are ‘trapped’ at the lateral border of the rectus abdominis muscle. It may follow previous surgeries on the abdomen but sometimes a cause is not found.
What are the symptoms?
Pain is experienced near the middle of the abdomen usually on one side only and, while usually localised, it may radiate between the lower border of the ribs down to just above the groin. The pain is not related to any gastrointestinal symptoms such as diarrhoea, constipation or other altered bowel habit with or without weight loss. It may be related to movement or exercise. The prevalence of the syndrome is said to range between 15% and 30% depending on the definition and the diagnostic criteria that is used. In adolescents, it is reported to be diagnosed in one out of eight cases of chronic abdominal pain. In the emergency department, the prevalence of ACNES in the patients presenting with acute abdominal pain has been reported to be a mere 2% of cases as usually there is the presence of a serious acute pathology in such patients.
Clinically when examining a patient, pain at the point of tenderness can be palpated when the abdomen is soft and if the patient is asked to ‘sit up’ and hold this position i.e tensing the abdominal muscles; if this makes the pain worse then this is a positive Carnett’s test and more in keeping with ACNES, if not then the test is negative.
It is important to exclude an underlying abdominal or gastrointestinal condition before the diagnosis of ACNES can be made.
In summary, diagnosis can be made when a patient presents with the following as described below (although not all need to be present)
- Unilateral locoregional pain at the abdominal wall lasting for at least 1 month
- The presence of a unilateral tender spot at the abdominal wall (a trigger point of <2 cm2 fingertip area of maximal tenderness, localized at the lateral border of the rectus abdominis)
- A positive Carnett’s test
- A positive skin pinch test and/or altered skin perception to light touch and/or cold at the area of the most intense pain
- Normal laboratory findings with no indication of inflammation or infection, and in the absence of any surgical cause of pain
- Negative imaging of the abdominal wall
- Temporary positive relief in pain response after injecting a local anaesthetic (usually lidocaine) at the diagnostic trigger point
Treatment options
Investigation may initially be managed by a gastrointestinal specialist clinician to ensure that there is no other pathology present, which may account for the abdominal pain experienced; this may involve the use of endoscopic examinations, a CAT scan of the abdomen as well as blood tests. Injections into the muscles/nerves at the affected site of pain, can also aid in pain relief and also may confirm and diagnose the condition. Treatment such as pulsed radiofrequency will be often offered when these injections are positive, and is described below. Pain killers may be used in a step wise fashion and rely on the consultation and expertise of a pain specialist. Some of the painkillers used may be quite strong and lead to a patient becoming constipated, so the use of laxatives is sometimes also required. Chemical treatment by using various ‘injections’ in some cases with stronger agents such as botox also shown to have result.
Pain Medicine specialists may suggest ‘pulsed radiofrequency’ which involves using ultrasound to place an electrical probe between the muscles in the abdominal wall where the nerves lie. Once the position is correct then an electrical treatment is provided to the nerve to attempt to reduce the pain, without burning or damaging it.
Surgery: Generally relies on the use of a small incision just at the point of the pain and dividing the nerves that pierce the abdominal wall to supply the overlying skin (cutaneous nerves). This procedure is undertaken with the patient asleep (under general anaesthetic). The procedure will leave a scar and may be undertaken as a day case.
This procedure is performed by Consultant Hernia and Groin Surgeon Professor Aali Sheen.
Managing the pain
Once a diagnosis is made a management plan can be considered. Initially injecting a local anaesthetic (usually lidocaine) at the diagnostic trigger point provides a temporary relief in pain response for at least by 50% or more individuals and can be helpful in making the diagnosis and has been reported to provide long term relief. Painkillers can be used and may include pain medication which is specifically designed for nerve pain such as amitriptyline and gabapentin as well as the use of anti-inflammatory medication. A pain specialist can assess and guide on the prescription of these medications as well closely following up how effective the medication is in controlling the pain experienced.
In summary, pain can be managed in a multidisciplinary fashion, which is key for any individual presenting with ACNES and relies of the use of painkillers, injections and potentially for consideration of surgery. Surgery is not frequently carried out but is usually managed by a peripheral nerve surgeon or abdominal wall specialist surgeon.
Evidence/ Success
Large centres carrying out the operation for ACNES have shown good results and quote a 70% success rate at one year. Some studies have shown pain free results in 86% of patients with over 75% experiencing long-term success. About 2/3rd of patients do get better with an improvement in their quality of life as well a reduction in the use of as well as in many cases cessation of pain killers they are taking. Other recommended treatments include pulsed radiofrequency ablation and localised injections as described above.
Treatment description
- Pain killers including morphine in some cases
- Trigger point injections and nerve blocks around the site of pain
- Pulsed radiofrequency ablation
Recovery and rehabilitation
It is important to ensure that you receive good rehabilitation advice from your treating clinician and if you have seen a physiotherapist in the past it is worth continuing with some physio and rehab after your treatment.