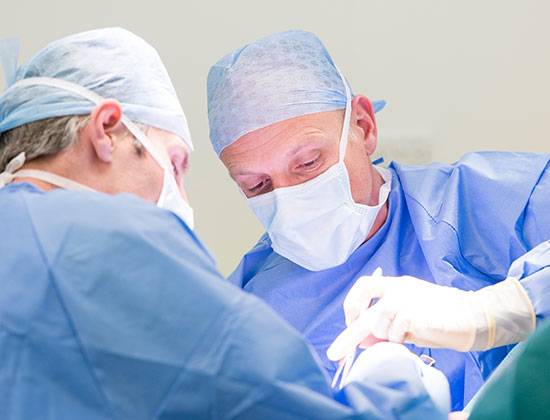
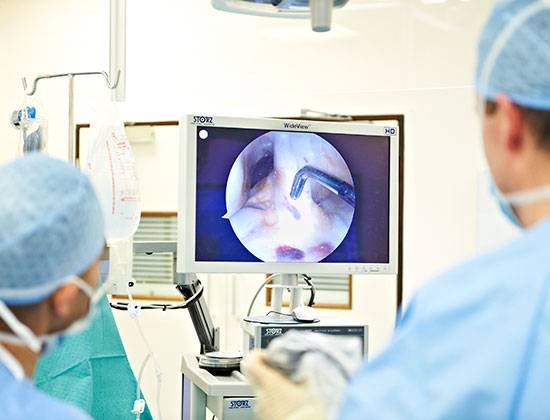
My Mako Knee Replacement
9 July 2018
An active life
Jo had always been active, a competitive swimmer at a young age, she’d seen numerous physios as a teenager for her ‘breaststroke knee’, something she puts down to the 70s and 80s school of thinking of ‘no pain no gain!’ During her twenties she took up competing in triathlons and marathons and mountain marathons, while working as a policewoman for many years, walking the beat for up to eight hours at a time, and a 12-mile round cycle commute. By the time Jo reached her mid-thirties, she began to wind down her activity due to ongoing issues with her knee. She was able to do less and less, even indoor spin classes hurt her knee too much, and gradually she found she couldn’t do the sports she loved. Years of intensive physiotherapy to help with muscle strength and imbalances enabled her to do some of the activities she enjoyed, but this came at a price; living in constant pain.
Enough was enough!
A regular commute throughout London and the Home Counties meant Jo was often on her feet and walking long distances, something she enjoyed and often took hiking holidays. However, it wasn’t until a walking holiday in the UK, on more gentle terrain where Jo found she couldn’t keep up with friends that she decided she needed to seek help for her knee.
Jo saw a private consultant who referred her for an MRI scan. This confirmed arthritis in her knee, and no protective cartilage to help cushion the bones, which had started rubbing together. Her doctor recommended a full knee replacement with multiple injections and other treatments alongside. Talking this through with friends at Christmas, Jo was recommended to get in touch with Jonathan Webb at Fortius by a friend.